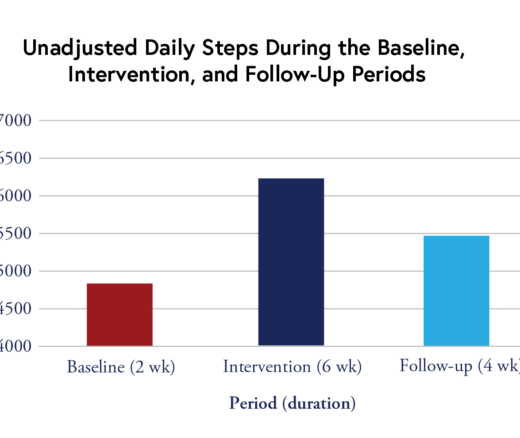
A Simple, Gamified Program Boosted Walking in Parkinson’s Patients
Chart of the Day: Remote Intervention with Gaming Elements Shows Promise, LDI Expert Finds
Improving Care for Older Adults
Blog Post

This summer, when Washington state begins paying the first long-term care insurance benefits to residents, it will mark the public debut of an audacious experiment. A single state is going where the federal government fears to tread.
The effort, which relies on small payroll taxes, will fund a $36,500 lifetime benefit for each qualifying resident. While the benefit is small, the state continues to innovate by allowing private insurers to create supplemental policies that make the product more robust.
The state’s program, WA Cares, could become a model for the country or a spectacular failure—or something in between.
Either way, LDI Senior Fellow Norma Coe will be watching. The health policy professor at the Perelman School of Medicine poses many questions below for new research angles.
Public long-term care insurance already serves most European countries, Coe notes, but it remains a deferred dream in the U.S. A national program—designed to help pay for assistance with daily activities at home or in nursing homes—was part of the original Affordable Care Act but suffered from several design and implementation flaws and was scuttled for its high costs before launch.
The market for long-term care insurance—never strong—has been weakening further since the pandemic. People who purchase it complain of having to pay ever-rising premiums or lose all coverage. Medicaid covers the very poor, but everyone else must fend for themselves. The average 65-year-old will pay $120,000 over their lifetime for care, representing the largest health expense most of us will ever face, an LDI brief notes.
Coe has been intrigued by long-term care and its insurance (LTCI) since graduate school when she worked with Amy Finkelstein of MIT and Jeffrey R. Brown of the University of Illinois.
Coe’s recent paper with Courtney Van Houtven and Gopi Shah Goda—on the spillovers to family members on LTCI—is among her best-known papers in this area. At the same time, her original paper, “Medicaid Crowd-Out of Private Long-Term Care Insurance Demand: Evidence from the Health and Retirement Survey,” remains her most cited on LTCI.
Check out more from Norma Coe below:
Coe: The private LTCI market has been contracting since the COVID-19 pandemic. Long-term care, as opposed to curative care, is simply left out of health insurance policies in the U.S., except for Medicaid, where there are strict financial limits on eligibility, or within the Veterans Affairs (VA) program.
Washington State is the first to pass and start a public long-term care insurance program for state residents, although it is admittedly a small policy.
Coe: Many other countries have more generous LTCI coverage in their public insurance systems. I think some LTC expenses could be insured through a public insurance program, and doing so would likely strengthen the economy.
Coe: This paper documents a new reason why long-term care insurance take-up is low: the mismatch between decision-making power and long-term care risk. We see that when married women have more power in health care decisions, specifically, there is a higher likelihood that they have private long-term care insurance. However, just giving married women more bargaining power won’t solve the problem. This is just one of a host of reasons why we see low long-term care insurance take-up rates, a long-standing research topic in the economics literature. This body of work highlights the difficulties in relying on voluntary LTCI coverage to shift the risks people face.
Coe: I’d love to see more work thinking about public options and benefits. We essentially have catastrophic coverage through Medicaid, but the lack of a long-term care financing and delivery system has implications for care received and labor force decisions of adult children.
Coe: As the first state to institute this program, or anything like it, there is so much to watch! It has been highly controversial since its passing, so many residents know about the program. What will it do to people’s expectations for who will provide long-term care? How will it affect savings decisions? The workforce? Beneficiaries and the care they receive? Medicaid enrollment? The overall financial risk people face? And the economy?
Coe: I don’t think there is one country alone we should look at – as each is unique to fit their cultural context, and many are wrestling with how to address the baby boom generation’s upcoming needs with limited resources. That said, Germany and the Netherlands are two systems I keep my eye on.
Coe: I’m hoping to look closer at the WA Cares program and its effects on care providers, expectations, and beneficiaries, as well as the overall LTCI market. I also want to continue my work that tries to identify and measure the relative benefits of various LTC delivery models to help inform what we might want policy to incentivize and insure.
The article, “Long-Term Care Insurance Within Married Couples: Can’t Insure One Without the Other?” was published on May 23, 2025 in Review of Economics of the Household. Authors include Norma B. Coe, R. Tamara Konetzka, Chuxuan Sun, and Courtney Harold Van Houtven.


Chart of the Day: Remote Intervention with Gaming Elements Shows Promise, LDI Expert Finds

Penn LDI Panel Cites Costs for Enrollees Alongside Billions in Overpayments and Systemic Gaming

New Evidence Undercuts Industry Warnings and Supports the Case To Restore Federal Minimum Staffing Standards

Issue Brief: Understanding Gaps and Opportunities to Advance Research and Policy

An LDI Fellow Draws on Historic, Paradigm-Shifting Treatments in Depression and Obesity to Consider What Meaningful Breakthroughs in Dementia Care Could Look Like

A Penn LDI Virtual Panel Looks Ahead at New Possibilities