Health Care Access & Coverage | Health Equity
Blog Post
How Anti-Immigrant Rhetoric Affects Health Care Utilization: Chart of the Day
Primary Care Utilization Declines as Anti-Immigrant Sentiment Rises
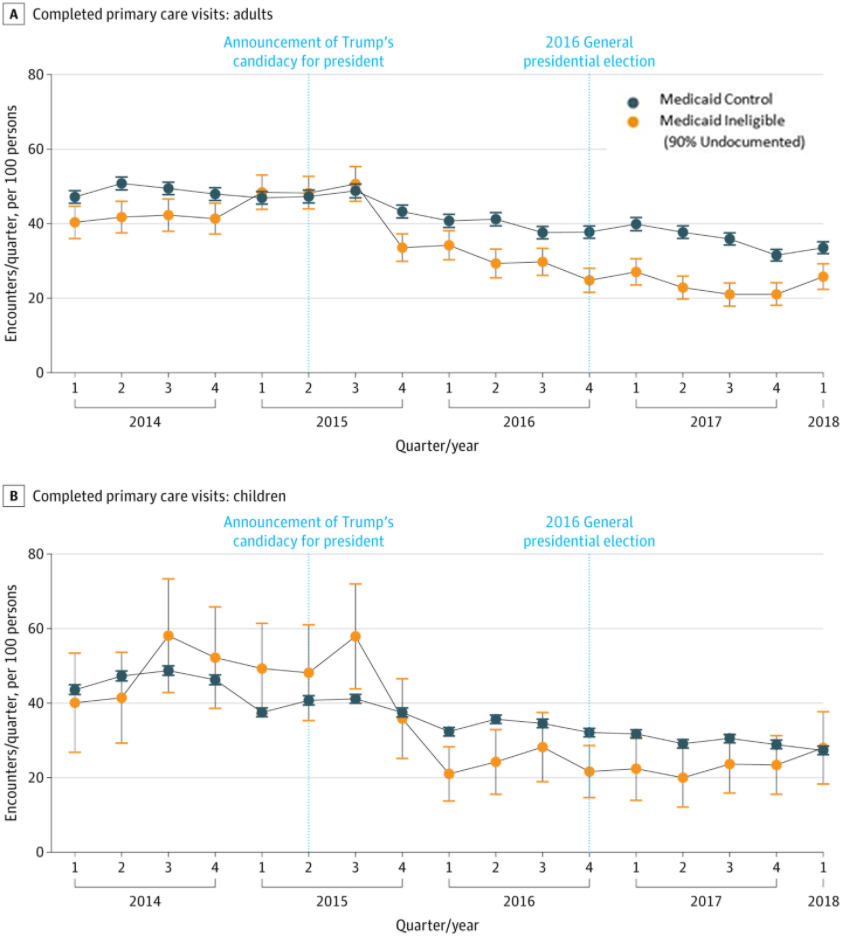
The 2016 presidential campaign saw a dramatic rise in anti-immigrant rhetoric. The sudden, high-profile change was associated with a substantial decline in utilization of health care services by undocumented adults and their children, as shown in the above chart. That’s the takeaway message from a new study in JAMA Network Open by former LDI Associate Fellow Joseph Nwadiuko and colleagues.
The authors compared primary care visits, emergency department use, and inpatient discharges from 2014 through 2017 for more than 20,000 patients in the Johns Hopkins Health System (JHHS), drawing from The Access Partnership (TAP) program. TAP cares for low-income patients who are ineligible for Medicaid, in large part due to immigration status—92% of TAP participants are undocumented. The authors compared utilization and outcomes to Medicaid patients in eight Medicaid plans in Maryland.
From the announcement of Donald Trump’s candidacy in June 2015 through May 2018, there was a 43.3% relative decrease in primary care visits for undocumented children and a 34.5% relative decline in undocumented adult primary care visits. Emergency department use increased for undocumented children, and there was a relative decrease in hospitalizations among undocumented adults.
The decreases stabilized—but did not reverse—in the fall of 2016, suggesting a bottoming out of the effect. However, the authors note that no-show rates continued to fall after 2016, suggesting the chilling effect may have continued in other ways. This study aligns with similar research from Illinois in Houston and builds a case that sustained anti-immigrant rhetoric may have raised fear of discrimination and deportation when encountering health care systems. Notably, undocumented persons have high rates of posttraumatic stress, which often presents as hypervigilance. Furthermore, the lack of changes in use by Hispanic and Latinos patients with documentation suggests the effect is specific to the undocumented population.
The Leonard Davis Institute of Health Economics partially funded this study through a pilot grant.
The study, Trends in Pediatric Emergency Department Utilization after Institution of COVID-19 Mandatory Social Distancing was published in JAMA Network Open on March 5, 2021. Authors include Joseph Nwadiuko, Jashalynn German, Kavita Chapla, Frances Wang, Maya Venkataramani, Dhananjay Vaidya, and Sarah Polk.