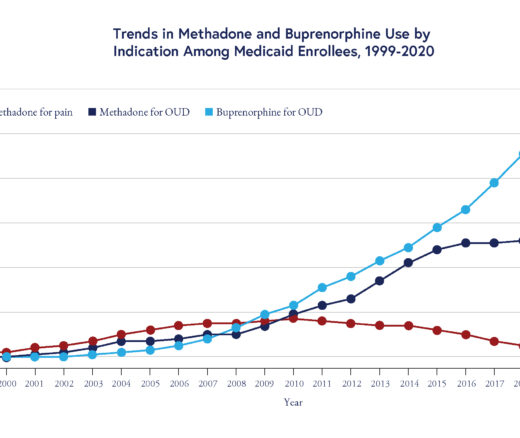
Methadone Use Rises—But Too Few People Get Opioid Medication
Chart of the Day: Methadone Use for Opioid Use Disorder Tripled From 2010–2020, Yet Only One in Four People With Addiction Receive Medication
Substance Use Disorder
Blog Post
This post was originally published in December 2019 and covered the study when it was released as an NBER Working Paper. It has now been updated to reflect its publication in The Quarterly Journal of Economics.

A state prescription drug policy first adopted in 1939, and last ended in 2004, appears to have influenced where Purdue Pharma chose to market its opioid drug OxyContin upon launch in 1996. The consequences of that decision reverberate to this day, according to a new study in The Quarterly Journal of Economics by LDI Senior Fellow Abby Alpert and colleagues, who estimate that states with the prescription policy had 11.3 fewer overdose deaths per 100,000 people in 2017. Let that sink in for a moment. In 2017.
The paper is a rigorous and tantalizing analysis of how public policy can influence and interact with commercial activities, leading to effects that could not be foreseen upon enactment of the policy. In the context of the opioid epidemic, these effects have had enduring impact on overdose deaths in the subsequent generation. These results are compelling evidence that the introduction and marketing of Oxycontin explain a large share of the overdose deaths in the last 20 years.
The policy was an early prescription drug monitoring program that required physicians to use a state-issued triplicate form when prescribing Schedule II controlled substances (which includes many opioids). The physician had to keep one copy on record. The patient took two copies to the pharmacy; the pharmacy kept one and sent the third copy to the state drug monitoring agency. The state agency maintained a database from these forms to monitor and investigate prescribing irregularities and diversion. California was the first state to adopt a triplicate prescription program, followed by Idaho, Illinois, Indiana, Michigan, New York, and Texas between 1961 and 1988. Not surprisingly, all these programs eventually ended with the advent of electronic monitoring systems.
Enter Purdue Pharma, eager to market its new drug OxyContin in 1996. Triplicate programs had been effective in reducing prescribing of the drugs subject to the policy, due to physician concerns about tangible government oversight of their prescribing behavior and the hassle factor in handling and keeping records of the triplicate forms. Five states had a triplicate program in effect when Purdue Pharma crafted its marketing strategy (Indiana and Michigan had already ended their programs.)
“Triplicate states” are mentioned repeatedly in Purdue Pharma internal documents as having been important barriers to OxyContin prescribing, with lower expected returns from marketing spending. These documents suggest that less marketing was targeted to triplicate states, with one document recommending that “the product [OxyContin] should only be positioned to physicians in non-triplicate states.” Indeed, triplicate states had some of the lowest OxyContin adoption rates in the country.
Alpert and colleagues find that the marketing practices of OxyContin interacted with state policy and led to dramatically reduced overdose death rates in triplicate states. By comparing trends in triplicate vs. non-triplicate states, they provide empirical evidence that the origins of the opioid epidemic lie in the marketing of OxyContin. As shown in Figure 1, these differences became more pronounced as time went on, consistent with the ramp up in sales of OxyContin and time involved in transitioning from use to misuse and dependence.
By deterring the introduction of OxyContin, triplicate states were largely protected from the fatal overdose trends in the rest of the nation. Using these results, the authors estimate how many opioid overdose deaths can be explained by the differences in exposure to OxyContin’s launch and marketing between triplicate and non-triplicate states. If non-triplicate states had the same initial level of exposure to OxyContin as triplicate states, they would have had 34% fewer drug overdose deaths and 45% fewer opioid overdose deaths on average each year from 1996-2017. The new study provides the first quasi-experimental evidence on the initial causes of the opioid crisis, and is worth a full read.
The study, Origins of the Opioid Crisis and its Enduring Impacts, was published online in The Quarterly Journal of Economics on November 13, 2021. Authors include Abby Alpert, William N. Evans, Ethan M. J. Lieber, and David Powell.

Chart of the Day: Methadone Use for Opioid Use Disorder Tripled From 2010–2020, Yet Only One in Four People With Addiction Receive Medication

LDI Fellows Used Medicaid Data to Identify Individuals at Highest Risk for Cocaine- and Methamphetamine-Related Overdoses, Paving the Way for Targeted Prevention

Penn and Four Other Partners Focus on the Health Economics of Substance Use Disorder

Penn Medicine’s New Summer Intern Program Immersed Teens in Street Outreach Techniques

LDI Experts Offer 10 Solutions to Get More Help to Seniors With Addiction

More Flexible Methadone Take-Home Policy Improved Patient Autonomy