
New Rules for Methadone Doses at Home Did Not Increase Overdoses
More Flexible Methadone Take-Home Policy Improved Patient Autonomy
Substance Use Disorder
Blog Post
The alarming rise in drug overdoses has been uneven in the U.S., with significant disparities across urban neighborhoods. In a new study, we examine whether the presence of alcohol outlets contributes to neighborhood disparities in drug overdoses, and whether alcohol outlets that sell drug paraphernalia are associated with neighborhood overdose rates.
The study, published in International Journal of Drug Policy, found that each additional off-premise alcohol outlet in a Baltimore City neighborhood was associated with a 16.6% increase in the neighborhood drug overdose rate. Off-premise settings include liquor and package stores and taverns that sell liquor, beer, and wine. In contrast, on-premise alcohol outlets (restaurants, bars, hotels, and entertainment venues) were not significantly associated with the neighborhood overdose rate when off-premise outlets were also present in a neighborhood.
Why did we focus on alcohol outlets? A large body of literature has linked off-premise alcohol outlets with drinking problems, crime, and violence. Unlike on-premise outlets, off-premise alcohol outlets can sell alcoholic beverages in large quantities to patrons who are unmonitored by servers and often drink in nearby, uncontrolled environments, such as motor vehicles, parking lots, or street corners. Consequently, off-premise outlets are often surrounded by signs of alcohol consumption and signals of social disorganization, such as empty or broken bottles, loiterers, and publicly intoxicated patrons. Because these areas are often located in communities with low social capital and collective efficacy, they may be opportune locations for illegal drug sales. More alcohol outlets are generally found in economically depressed, predominantly-minority neighborhoods, exacerbating health disparities in these communities.
To further examine the connection between alcohol outlets and drug overdoses, we visited every off-premise alcohol outlet in Baltimore City and measured drug paraphernalia items for sale. Paraphernalia included items used to distribute or sell drugs (e.g., baggies, scales); items used for drug inhalation (e.g., pipes, hookahs, bongs, vaporizers, e-cigarettes); and unregulated synthetic drugs, such as synthetic cannabinoids. We found that as the proportion of off-premise outlets selling drug paraphernalia went up, neighborhood overdose rates went down:
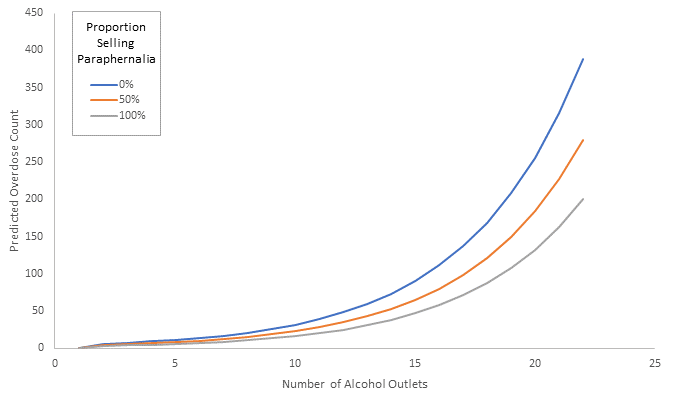
This finding may be counterintuitive. One explanation is that we measured overdose rates by EMS-911 calls, and that might have had an impact. Because drug markets develop around alcohol outlets in low-resource neighborhoods, increased policing of these locations may negatively affect 911 calls for drug overdose. Studies show that drug arrests cluster around alcohol outlets, indicating increased policing around these establishments. In heavily-policed environments, people who use drugs and other bystanders may be wary of calling 911 in the event of an overdose. Even if a bystander has not been using drugs, mistrust of the police and fear of repercussions of police contact, such as lost housing and child custody, social stigma, and repercussions from local drug dealers may deter 911 calls for drug overdose. It is also possible that a different data source (such as fatal drug overdoses from a medical examiner case archive) might produce different results.
This study, to our knowledge, is the first to link off-premise alcohol outlets to drug overdose rates. It suggests that alcohol outlets, particularly those that sell drug paraphernalia, could be community partners for harm reduction strategies, such as naloxone distribution or health communication on drug purity or identifying overdose symptoms. Alcohol outlets may also be potential focal points for community outreach and education campaigns around Good Samaritan Laws to encourage bystander support for drug overdose.
The study, Alcohol Outlets, Drug Paraphernalia Sales, and Neighborhood Drug Overdose, was published in the September 2021 edition of the International Journal of Drug Policy. Authors include Elizabeth D. Nesoff, Adam J. Milam, Christopher Morrison, Brian W. Weir, Charles C. Branas, Debra M. Furr-Holden. Amy R. Knowlton, and Silvia S.Martins


More Flexible Methadone Take-Home Policy Improved Patient Autonomy

Pediatricians’ Suggestions for Health Care Providers, Institutions, and Policymakers

Pain Is Hard to Predict, and a Cheap Disposal Kit Offers a Solution

New Geographic Trends Raise Questions About the Future of Behavioral Health Services

This Model Is Cheaper And Easier To Use Than The ER, LDI Fellow Argues In New Op-Ed