
Experts Warn Addiction Policy is Weak Despite Falling Overdose Deaths
Penn LDI Panel Urges Family-Focused Strategy and Stronger Health System Response
Substance Use Disorder
Blog Post
It’s the worst part of my job as an emergency physician: witnessing how the pandemic has widened gaps in care for people struggling with substance use disorders (SUD). These gaps have resulted in thousands more overdose deaths since 2020. But that’s population data; there’s only one real statistic to the parents of a young adult suffering an accidental fentanyl overdose. “Accidental” refers to unpreventable, like a tsunami, and overdoses are preventable. If only my patients had been able to access care while in the chaos of addiction.
On April 12, 2022, the Pennsylvania House Health Committee hosted a public hearing on opioids in the commonwealth. The goals were to update lawmakers on the challenges of the rising death rate from fentanyl and other synthetic substances and to encourage clinicians, advocates, and state leadership to advance possible solutions. My testimony at this public hearing focused on the need to expand (1) low-barrier treatment access (via emergency department [EDs], peer-led engagement, and telehealth) and (2) harm reduction strategies (via naloxone, fentanyl test strips, and syringe service programs).
Multiple studies, including randomized controlled trials, have demonstrated the efficacy of medication-for opioid use disorder (MOUD); buprenorphine, especially, is arguably a more effective treatment for SUD than aspirin is for heart disease. Unfortunately, medications are underutilized due to provider- and patient-level barriers to treatment access that foil the best intentions. Appointments, insurance, transportation, and pharmacies can all stand in the way of the first dose of this life-saving medication.
Several state and local organizations have collaborated to lower these barriers to care delivery. Initiatives include mobile vans that offer treatment in communities and EDs that provide 24/7 medication initiation by clinicians. These ED clinicians have received special training that empowers them to combat the addiction cycle by engaging patients during the ED visit.
And now, we also have telehealth as another point of access for treatment. During the early pandemic, prior requirements for in-person buprenorphine prescribing were rapidly replaced with the option to provide low-barrier addiction care via telephone. Telehealth has created a critical safety net that is more convenient than the ED and more patient-centered than typical care settings, including allowing privacy from the real or self-stigma of addiction clinics or substance use treatment centers.
In Pittsburgh, a telehealth clinic launched in April 2020 has initiated over 800 patients on buprenorphine. In Philadelphia, our CareConnect warmline—through funding from the Philadelphia Department of Public Health and in partnership with Penn Medicine on Demand—offers free telehealth substance use navigation and same-day buprenorphine. In rural areas where there are provider shortages, telehealth can solve the problem of long appointment waiting times for addiction care.
A statewide network of telehealth “addiction bridge” treatment options is paramount to prevent gaps in care and continue patients on medication during transitions from hospital to outpatient, incarceration to release, and pregnancy to parenting. We must sustain current exceptions to federal regulations for telehealth and create billing parity for services provided via telehealth or in person. We also need to develop culturally informed treatment programs to better meet the needs of different populations. For instance, fatal overdoses in communities of color increased 30% in the Philadelphia area in 2020. These disparities can be addressed with tracking of medication use and the application of harm reduction tools. Telehealth and ED care may provide some of these gateways to treatment.
In 2018, the Pennsylvania Department of Human Services developed a measure to incentivize follow-up treatment after ED visits for opioid use disorder. Through the Medicaid Hospital Quality Improvement Program (HQIP), Pennsylvania EDs engaged patients in treatment by prescribing buprenorphine and making a warm handoff to a local treatment center. This program can be expanded throughout Pennsylvania using a model, similar to one implemented in California EDs, that would expand the program so that every ED in the state could provide buprenorphine and naloxone, coupled with transitions to ongoing care and sustainable recovery. Implementation can occur across Pennsylvania now that the HQIP program has matured and various successful ED buprenorphine programs can serve as models for EDs that have not yet begun offering treatment initiation.
We have developed programs utilizing the wisdom of peer recovery specialists—people in recovery from opioid use who build alliances with patients and help them navigate the early treatment journey. Peers provide a pathway to sustainable employment for people with substance use experiences while also providing patients with emotional support. We can expand this element of the treatment paradigm by developing billing and reimbursement strategies for these services that can be initiated in EDs and in primary care and obstetric practices.
Increased syringe services programs would be a powerful tool in the fight against SUD, helping to reduce HIV and hepatitis C. Senate Bill 926 would legalize syringe services programs in Pennsylvania. These programs have been successful in Philadelphia and Pittsburgh, and expanding them to the rest of Pennsylvania will save millions of dollars and reduce the burden of these chronic infections. Syringe services programs function as community havens and gateways to treatment services and as resources for harm reduction education and resources.
We lose 15 Pennsylvanians every day to opioid use. These are my patients and families. We need innovation and rapid action to implement accessible treatment throughout the state.


Penn LDI Panel Urges Family-Focused Strategy and Stronger Health System Response
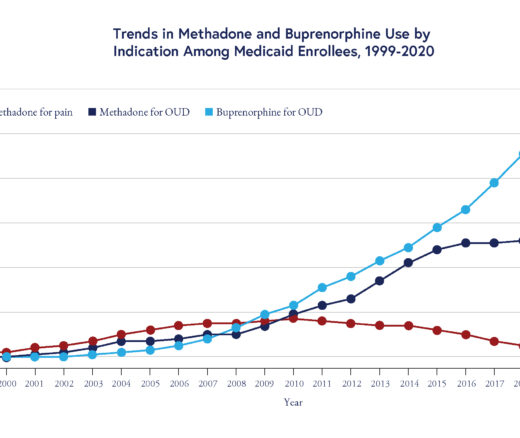
Chart of the Day: Methadone Use for Opioid Use Disorder Tripled From 2010–2020, Yet Only One in Four People With Addiction Receive Medication

LDI Fellows Used Medicaid Data to Identify Individuals at Highest Risk for Cocaine- and Methamphetamine-Related Overdoses, Paving the Way for Targeted Prevention

Penn and Four Other Partners Focus on the Health Economics of Substance Use Disorder

Penn Medicine’s New Summer Intern Program Immersed Teens in Street Outreach Techniques

LDI Experts Offer 10 Solutions to Get More Help to Seniors With Addiction