
U.S. Children Are Suffering: A Generation Grows Up Sicker, Sadder, and Dying Sooner
From Anxiety and Loneliness to Obesity and Gun Deaths, a Sweeping New Study Uncovers a Devastating Decline in the Health and Well-Being of U.S. Children

From Anxiety and Loneliness to Obesity and Gun Deaths, a Sweeping New Study Uncovers a Devastating Decline in the Health and Well-Being of U.S. Children

Chart of the Day: National Study Shows White Patients More Likely Than Black Patients to Get CT and/or Ultrasounds for Abdominal Pain in the Emergency Department
Hospitals and Physician Groups Can Also Benefit From Those Payments, as Medicare Launches a New Model for Episodic Care

LDI Experts Offer 10 Solutions to Get More Help to Seniors With Addiction

With MA Now Covering Over Half of U.S. Seniors, Researchers Face Flawed Data That Can Distort Results

LDI Fellows Uncover Six Key Barriers and Solutions to Achieving Better Hospital Care

This Social Media Tool to Fight HIV Could Be Scaled up to Help Local Health Officials, LDI Experts Say

New Findings Highlight the Value of 12-Month Eligibility in Reducing Care Gaps and Paperwork Burdens
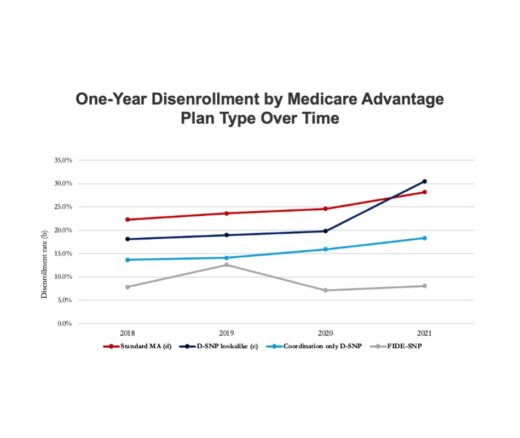
Chart of the Day: Fully Integrated D-SNPs Kept These Vulnerable Patients Enrolled, a New Study Finds

Mandated Nurse-to-Patient Ratios Have Cut Deaths, Eased Burnout, and Saved Millions. Policymakers Must Act Now to Protect Patients

These Five Strategies Can Make Surveys More Impactful, Says Wharton/LDI’s Ingrid M. Nembhard
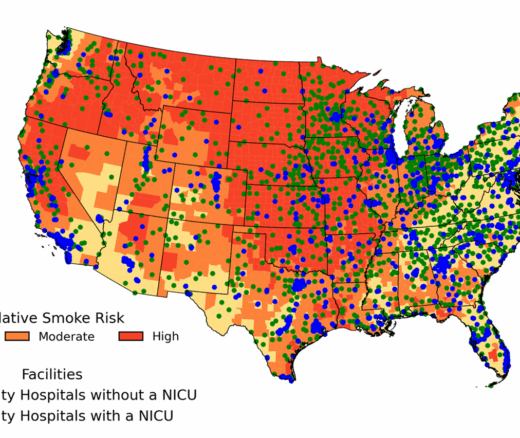
Chart of the Day: New Study Maps Maternity Care Gaps in Smoke-Prone U.S. Counties