
Over 500 U.S. Hospitals Have Stopped Delivering Babies Since 2010
A Crisis in Maternal Care is Unfolding—and it’s Hitting Rural and Urban Communities Alike
Blog Post
Millions of U.S. adolescents lost reproductive autonomy after the Supreme Court overturned the constitutional right to abortion in June 2022. The federal Title X program, which allows minors to consent for and access confidential family planning care and other reproductive services, can minimize the harmful effects of this reversal. However, many clinics left the Title X program in 2019 following a rule change that required them to be physically and financially separate from abortion services and to not discuss or refer patients for abortions. This is even though the Title X program has never funded abortions.
In a recent JAMA Network Open study, my coauthors and I mapped Title X-funded clinics before and after the rule change and found a net loss of 1,249 clinics. As a result of this dramatic change to the Title X program, adolescents living in 8.7% of census tracts lost access to confidential reproductive health care. The research is gaining attention in the policy world, with CHOP PolicyLab writing about it and The Hill publishing a related op-ed.
We found that in 2020, 1.8 million U.S. adolescents aged 15-17 did not have access to confidential family planning care within a 30-minute drive (Figure 1)—more than twice as many as before the 2019 Title X rule change, according to census tract analysis. More than a quarter of adolescents in that age range lacked access in 15 states—nine more states than before the change. Young people in the Midwest were more than twice as likely to lose access to confidential care compared to those in the Northeast. Young people in rural areas, compared to urban areas, were also more likely to lose access. Additionally, young people living in relatively less affluent and more diverse areas were less likely to lose access.
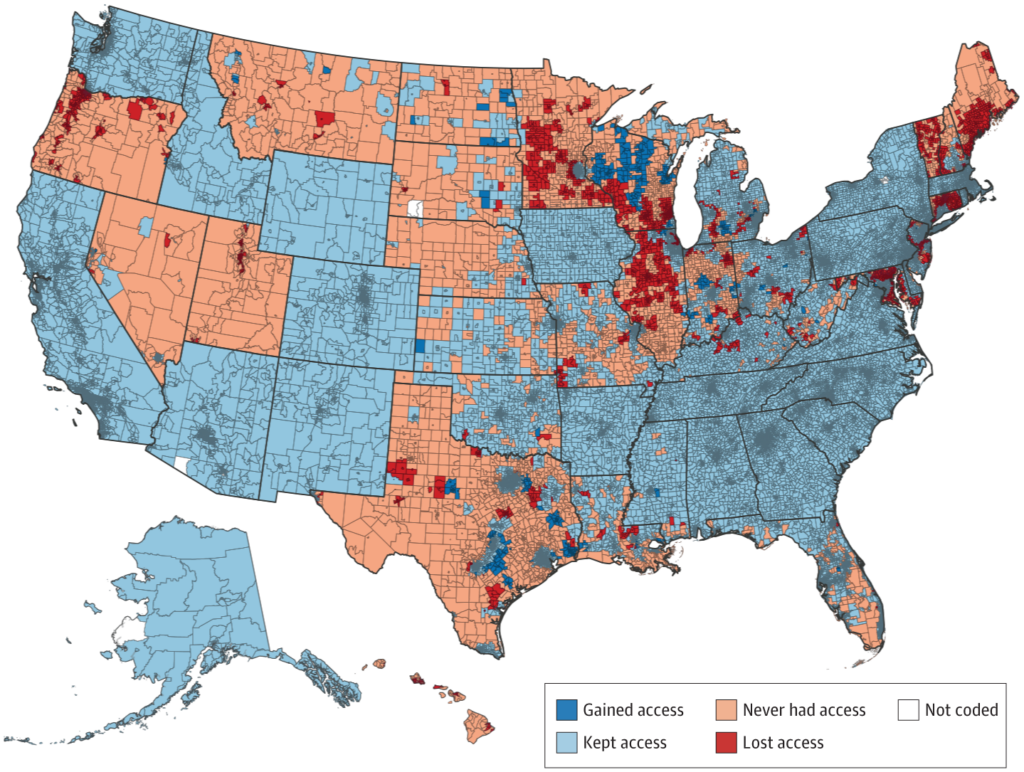
The 2019 changes to Title X were reversed in 2021, enabling previously funded clinics to reapply for the program. The program is working to rebuild. However, our data show that even if all the clinics rejoin the program, at least 880,000 adolescents aged 15-17 (6.4%) still may not have access to confidential reproductive care.
The science is clear: Adolescents need access to comprehensive sexual and reproductive health care. Expanding the Title X program is essential to ensure that all youth can access these services, particularly in regions where they do not have state-level reproductive health protections.
The Expanding Access to Family Planning Act, introduced in the Senate in July, is a critical step toward making this a reality. This legislation would provide 10 years of funding for the Title X program, allowing it to expand to reach all adolescents, and introduce protections to ensure that the regulations governing the program remain aligned with evidence-based practice.
States should also enact laws explicitly permitting all adolescents to consent for and be ensured confidentiality in obtaining sexual and reproductive health services. Clinicians in states where these laws are not currently enacted should familiarize themselves with Medicaid protections for confidentiality and work to ensure that Medicaid-enrolled youth are aware of their right to consent to reproductive care under Medicaid statutes.
Ensuring that all adolescents have access to the tools to prevent unintended pregnancy is a national priority. Our research indicates that protecting and broadening the Title X program is a critical step toward meeting that goal.
The study, “Adolescent Access to Federally Funded Clinics Providing Confidential Family Planning Following Changes to Title X Funding Regulations,” was published in JAMA Network Open on June 17, 2022. Authors include Polina Krass, Vicky Tam, Jungwon Min, Isabella Joslin, Lily Khabie, Tracey A. Wilkinson, and Sarah M. Wood.


A Crisis in Maternal Care is Unfolding—and it’s Hitting Rural and Urban Communities Alike

Stable Payments Improved Margins But Not Liquidity, New LDI Analysis Finds

LDI Senior Fellow Cited for “Significant Contributions” in Research

Outdated Laws Target Black and Queer Lives in Over 30 States, Fueling a Deadly Disease

Selected for Current and Future Research in the Science of Amputee Care

Research Memo: Delivered to House Speaker Mike Johnson and Majority Leader John Thune