Black Older Adults With Cancer Are Far Less Likely to Get Any Care
New Study From LDI and MD Anderson Finds That Black and Low-Income, Dually Eligible Medicare Patients Are Among the Most Neglected in Cancer Care
News

In an event that drew 10 dozen state and federal officials, university researchers, insurance executives, and health care organization managers to the University of Pennsylvania, the Leonard Davis Institute of Health Economics (LDI) and the Health Affairs journal held a July 22 conference focused on the integration of Medicare and Medicaid services for dual eligibles. The decades old issue remains one of health care’s most intractable problems.
In 1965, when Congress created the world’s largest public health insurance program and bifurcated it into two different systems—Medicaid and Medicare—legislative policymakers did not think much about how these two systems would ultimately overlap in the future.
Medicaid is essentially aimed at people of all ages who can’t afford to pay for medical care. Medicare is aimed at providing care to people over 65. Given its focus on low-income and marginalized populations, Medicaid has large groups of patients with severe disabilities and multiple chronic diseases. As these patients grow older and reach 65, they also go on Medicare, thus becoming dually eligible for the benefits of both systems. But the exact way in which that care should be delivered, funded, and managed between the two programs has never been comprehensively defined.
Medicare and Medicaid have different rules, regulations, requirements, restrictions, and procedures. These incompatibilities are further compounded by the fact that there are 50 different state Medicaid programs which are themselves often incompatible with each other. Inevitably, dual eligibles are often caught in a tangle of administrative inconsistencies and contradictions in a centerless duals system that prevents the delivery of needed care in ways that often result in catastrophic outcomes. Dual eligibles routinely face higher rates of hospitalization, emergency room visits, and other adverse health events due to the inefficiencies and gaps in a system that was essentially formed by accident rather than by evidence-informed and clearly thought-out policies and operational plans.
The Penn conference was the latest to assemble a corps of top experts to better understand how policymakers might forge a coherent path toward a model of fully integrated care for this highly vulnerable population.
As he opened the “Forging a Path Toward Integrated Care for Dually Eligible Individuals” conference, Alan Weil, JD, MPP, Editor-in-Chief of the Health Affairs journal noted that his nearly 30 years of involvement with dual eligibles has given him a deep historical perspective on the problems that continue to hobble the program.
“Integration is a challenge,” Weil said. “We have two programs with different rules, different governance, different financing, different cultures. None of that has changed. There is still the open question of who is the integrator? Ultimately, we want that to be some entity at the level of the patient, but how are we going to hold those entities accountable for what we’re trying to achieve with integration? Questions of accountability pivot around these systems having enough of the capacity to understand what’s going on so pressure can be placed on the system when needs are not being met. At the same time, the risk of handing this very complex problem over to any entity, particularly a managed care organization, without the infrastructure at the state and federal level or infrastructure at the consumer level, raises just tremendous risks. So, in 30 years, much has changed. But some of the fundamental questions really haven’t.”

One of the grimmest presentations about the country’s 13 million dual eligibles was that of Eric Roberts, PhD, an LDI Senior Fellow and Associate Professor at the Perelman School of Medicine. His research focuses on the delivery and financing of insurance and care for low-income Medicare and Medicaid individuals.
“Over half of dual eligible beneficiaries are people of color,” Roberts said. “More than 80% have complex multimorbidity, including diseases such as chronic kidney disease, diabetes, and hypertension. There are high rates of disability, cognitive impairment, and frailty. A third have serious mental illness. Over half report difficulty with one or more activities of daily living. Almost all have an annual income of less than $20,000 a year. And, an estimated 45% experience food insecurity as well as high rates of housing insecurity, and lack of transportation.”
“Dual eligibles account for about one-sixth of the Medicare population and one-seventh of the Medicaid population, yet they’re over 30% of the spending in both programs,” Roberts continued. “In 2021, total Medicare and Medicaid spending for these beneficiaries exceeded $490 billion. And there are concerns that much of the money is not purchasing high quality, efficient, and coordinated care, in part because the systems for managing care for this population are poorly configured for addressing complex needs.”
“The fact that Medicare and Medicaid are separately administered and financed raises concerns about the lack of integration potentially resulting in cost shifting or poor coordination of care across programs,” Roberts said. “There’s lots of evidence of cost shifting across the acute, post-acute, and long-term care settings and in other areas.”

Conference keynote speaker Toyin Ajayi, MD, MPhil, is the CEO of Cityblock, a health care provider that operates a network of 13 health centers running models of integrated care for Medicaid, dual eligibles, and low-income Medicare beneficiaries in seven states. She’s shown here on the conference stage with Rachel M. Werner, MD, PhD, Executive Director of LDI. Ajayi’s remarks focused intensely on the common daily experiences of dual eligible patients.
“Most dual eligible people have no single-entry point to access care and services. They have two insurance cards, and zero to five case managers—with all five trying to manage against different goals and priorities,” Ajayi said. “If they’re lucky, the patient might get a paid or family caregiver who tries to fill in the gaps. But even with the best of intentions across all these people, when there are so many disparate entities involved, it’s easy, maybe even inevitable, to point fingers elsewhere because no one’s accountable for anything.”
“For instance, someone needs a replacement wheelchair, so they call their durable medical equipment (DME) provider and submit an invoice to Medicare. But Medicare punts it to a Medicaid long-term services care provider payer who punts it back because it’s used within the nursing home grounds, which punts it back again, and the ping pong game just goes on and on. But in the middle of all this is a human whose experience is exhausting, precarious, and wildly inefficient. Days, then weeks, then months go by as this person goes without the right equipment and develops pressure ulcers from lying in bed all day—ultimately ending up in the hospital with sepsis from the wound,” said Ajayi.
“Whose job was it to prevent this inevitable event from occurring or to spare the patient the pain and distress and cost that we absolutely could see coming?” asked Ajayi. “This is basic stuff. If it is everyone’s responsibility, it’s actually no one’s responsibility. And that’s why integration and accountability are so important,” she said.

The conference’s “Perspectives of Dually Eligible Individuals” panel provided the diverse and pragmatic insights of dual eligibles individuals and caregivers. On stage were Rachel M. Werner, MD, PhD, LDI Executive Director and moderator; Dennis Heaphy, MPH, MEd, who appeared via a Zoom link; Aisha Adkins, MPA, CNP, a professional patient advocate; Dionne Stalling, Founder and Executive Director of the Rare and Black advocacy organization; Sharifa Abu-Hamda, Manager of the Independent Living Program in the Independence Care System; and Jean Minkel, Abu-Hamda’s personal caregiver.
“Too often in the current system, folks with complex needs are viewed exclusively as patients rather than people that spend the majority of their time living in the community, having families, working, and engaging in other social activities,” said Heaphy, a Health Justice Advocate and Researcher at the Massachusetts Disability Policy Consortium. “The services we really need are beyond directly medical, like addressing the social drivers of health—food, transportation, and other things. For instance, a wheelchair is not a medical device, it’s a means of getting around and maintaining your daily connections in the community. We need services that address isolation and loneliness. We need spiritual care that is never discussed in the literature. What’s needed is a system that focuses on the whole person as opposed to a list of medical diagnoses.”
“Policymakers need to adapt independent living philosophy and recovery model principles as part of the care that is provided,” Heaphy continued. “I require personal care attendants who support my ability to be a person engaging in the community. But in reality, now, personal care attendants are often assigned duties as medical providers in the home rather than as social support providers.”

The “State Options for Navigating Fully Integrated Care” panel was focused on the various ways that state Medicaid programs were managing how services for their region’s dual eligibles are handled. The moderator was Melanie Bella, MBA, Executive Advisor at Cressey & Company and former Chair of the Medicaid and CHIP Payment and Access Commission (MACPAC). The panelists were Matthew Behrens, MPA, Senior Policy Advisor for Complex Care and Duals Integration for the Virginia Department of Medical Assistance Services; Stacie Weeks, JD, MPH, Medicaid Director and Administrator of the Nevada Division of Health Care Financing and Policy (Zoom); Kelli Emans, Senior Strategic Integration Advisor for the Washington State Home and Community Services Division within the Aging and Long-Term Support Administration (ALTSA); Juliet Marsala, MBA, Deputy Secretary of the Office of Long-Term Living for the Commonwealth of Pennsylvania; and Anastasia Dodson, MPA, Deputy Director of the Office of Medicare Innovation and Integration at the California Department of Health Care Services (Zoom).
Explaining some of the ways services could be improved for dual eligibles, Pennsylvania’s Marsala said, “It’s important that we really get down in the weeds when we’re looking at changes Medicare could make for dually eligible patients. Sometimes solving small issues can have a tsunami effect. An example of one of those is with durable medical equipment stair glides where Medicare will only cover the cost of the motor. Everything else a patient needs to get and install a stair glide in their home must come from somewhere else, even with the Medicaid or private pay plan.”
“And then, the patient needs a care coordinator to figure out the really small details of getting all of that together, and that can be very cumbersome and difficult. Looking below the big picture, we need to see the layers and layers of boots-on-the-ground impact these things have and try to simplify and align those elements better. We could then see vast improvement as multiple small things build up to the practical operationalizing of the grander policies in ways that really get to the basics and make things simpler and better for patients.”


New Study From LDI and MD Anderson Finds That Black and Low-Income, Dually Eligible Medicare Patients Are Among the Most Neglected in Cancer Care

Her Transitional Care Model Shows How Nurse-Led Care Can Keep Older Adults Out of the Hospital and Change Care Worldwide
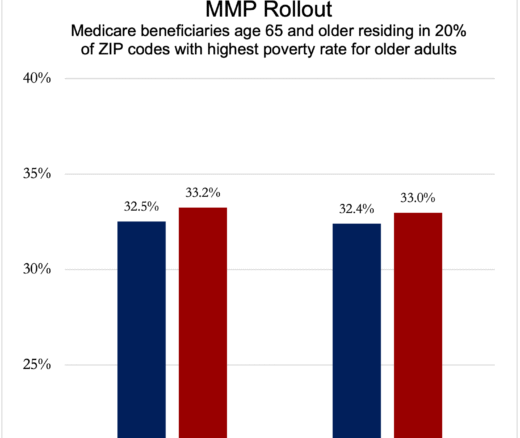
Chart of the Day: Medicare-Medicaid Plans—Created to Streamline Care for Dually Eligible Individuals—Failed to Increase Medicaid Participation in High-Poverty Communities

Penn LDI Debates the Pros and Cons of Payment Reform
Direct-to-Consumer Alzheimer’s Tests Risk False Positives, Privacy Breaches, and Discrimination, LDI Fellow Warns, While Lacking Strong Accuracy and Much More

One of the Authors, Penn’s Kevin B. Johnson, Explains the Principles It Sets Out