
Insurers Should Incentivize Non-Drug Treatments for Chronic Pain
An LDI Fellow and Chronic Pain Researcher Call on Health Plans To Lower Barriers to Physical Therapy, Acupuncture, and Interdisciplinary Pain Care
Blog Post
In 2014, Maryland transformed the way that its hospitals were paid. The goal was to increase the value of care delivered in hospitals —realigning incentives to improve quality while slowing growth in health spending. The experiences of a single state might seem too specific to be relevant elsewhere. However, a new study in JAMA Health Forum led by LDI Senior Fellow Austin Kilaru identified widely applicable lessons for value-based payment reform.

The Maryland All-Payer Model (MDAPM), developed in a partnership between the state and the Centers for Medicare & Medicaid Services (CMS), introduced global hospital budgets statewide. Instead of billing specified amounts for each item and service, hospitals were given high-level annual targets for expenditures and revenue, and flexibility in allocating resources. This approach was a major paradigm shift designed to move hospitals from fee-for-service strategies that reward high volumes of tests, procedures, and treatments, to preventing illness and improving quality.
MDAPM is estimated to have saved $916 million over projected spending through 2017. Quality improvements included reductions in unnecessary hospital admissions and readmissions. To determine if and how MDAPM might inform other payment reforms, Kilaru and his team interviewed 20 leaders involved in the design and implementation of MDAPM at the hospital, insurance, state, and federal level. Interviews focused on motivations, barriers, and facilitators for reform.
From the interviews, Kilaru and colleagues identified six major themes:
Kilaru views the lessons of MDAPM in two broad groups. Technical and logistical lessons included the use of data, the cooperative design process, and the reliance on communication. For example, a major challenge was setting budgets for each hospital. Federal and state policymakers needed precise data on health care utilization to work with individual hospitals to set budgets. Vigorous, detailed communication kept hospitals, payers, and other parties informed about adjustments and elicited valuable feedback.
Important strategic and cultural lessons also arose from the way that Maryland implemented this large, complex change. Although participation in the MDAPM was mandatory, Kilaru notes that buy-in from all participants was crucial. To make it easier for hospitals to take the plunge into global hospital budgets, the state and CMS set bold goals and high expectations but included transitional measures to soften the change such as maintaining revenue even as patient volume decreased. Hospital autonomy, with guardrails to prevent withholding care or extreme price changes helped secure buy-in. An external threat—the potential loss of a CMS waiver for previously implemented statewide price regulations—contributed to the commitment to change. Nonetheless, MDAPM created a collective sense that reform was visionary, in everyone’s best interest, and the right thing to do for patients.
One interviewee described MDAPM as a “monumental change” that “flipped the incentives for hospitals in the right direction.” Lessons from MDAPM have particular relevance to CMS reforms to increase financial stability and ensure access at rural hospitals. The Pennsylvania Rural Health model, currently in progress, is applying global hospital budgets to some rural hospitals. The goal is to reduce the pressure of competition with bigger hospitals by ensuring revenue and encouraging its use for community health initiatives. The national Community Health Access and Rural Transformation (CHART) model from CMS is funding rural communities to transform care delivery, including through global hospital budgets. These examples show how the findings from the Kilaru et al. study have the potential to guide hospitals, particularly in rural areas, as they transition to more sustainable, value-based financial models.
The study, “Health Care Leaders’ Perspectives on the Maryland All-Payer Model” was published February 4, 2022 in JAMA Health Forum by Austin S. Kilaru, Christina R. Crider, Joshua Chiang, Elisabeth Fassas, and Katherine J. Sapra.

An LDI Fellow and Chronic Pain Researcher Call on Health Plans To Lower Barriers to Physical Therapy, Acupuncture, and Interdisciplinary Pain Care
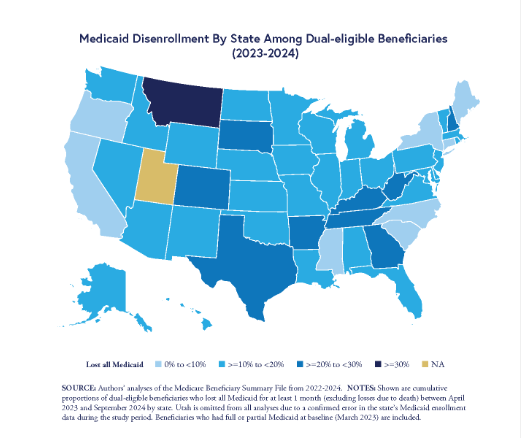
Chart of the Day: Researchers Urge Easier Renewals and Better Support To Prevent Gaps in Care

While They Wait for Medicare, People Approved for Social Security Disability Die at Higher Rates Compared to the General Public

Two Pediatricians Share Key Dates and Practical Next Steps

Medicare’s Payment Plan Can Ease Seniors’ Crushing Drug Costs but Medicare Buries it in the Fine Print
Even With Lower Prices, Medicare, Medicaid, and Other Insurers Tighten Coverage for Drugs Like Mounjaro and Zepbound Using Prior Authorization and Other Tools

Pandemic-Era Medicare Flexibilities Have Proven Effective, Popular, and Safe

A 2024 Study Showing How Even Small Copays Reduce PrEP Use Fueled Media, Legal, and Advocacy Efforts As Courts Weighed a Case Threatening No-Cost Preventive Care for Millions