
Health Care Affordability
Expert Insights
Blog Post

Outpatient surgery has become the “in” thing.
Most surgeries in the United States now occur outside the hospital, with more than 65% of procedures performed in outpatient settings.
The trend increased sharply during the COVID-19 pandemic and may have slowed afterward. But outpatient surgeries have continued to grow by about 6% a year and are especially common in orthopedics, eye surgery, and gastroenterology, according to a new study from LDI Fellows Angela T. Chen, Hummy Song, Guy David, and Alon Bergman.
By tracking multiple procedures over time, “Our study provides a more complete picture of how surgical care is evolving,” said Chen, whose team included Philip A. Saynisch and Aaron Smith-McLallen of Independence Blue Cross.
Over the next three years, federal regulators are phasing out the Inpatient Only List of surgeries that must be performed in a hospital, starting with 285 mostly musculoskeletal procedures in 2026.
The trends suggest a permanent shift to outpatient care, driven by new technology that allows complex surgeries, like joint replacements and spinal procedures, to proceed without a hospital stay, the authors said.
The team also found a significant equity gap in who benefits from the shorter recovery times that outpatient procedures provide. Patients in lower-income areas saw a 6% drop in outpatient procedures, while those in higher-income areas experienced a 5.2% increase.
Policymakers should monitor this trend and look for ways to reduce it, Chen said. Because outpatient surgeries cost less, patients should share in the savings through lower out-of-pocket expenses, the authors said.
Chen discussed more about the rise in outpatient surgeries below.
Chen: The regulatory environment is changing quickly, with the Centers for Medicare & Medicaid Services (CMS) finalizing a full phase-out of the “Inpatient Only” (IPO) list by 2028. These changes are intended to give surgeons more flexibility to choose the most appropriate setting based on patient needs rather than billing rules. Because Medicare often sets the standard for the broader market, these decisions tend to influence how commercial insurers and hospitals operate as well. Looking 10 years ahead, outpatient surgery will likely encompass even more complex cases as technology continues to reduce surgical risk and improve recovery at home.
Chen: We find that the pandemic-era shift toward outpatient surgical care persisted and deepened two years after elective surgeries resumed, suggesting a lasting change rather than a temporary disruption. Equally important is our finding related to equity: patients from lower-income areas experienced a 6% decline in procedure volume, while those in higher-income areas saw a 5.2% increase. By looking across multiple procedures and tracking patterns over time, our study provides a more complete picture of how surgical care is evolving.
Chen: For payers, the shift holds real promise – in our study, total costs for joint replacements fell by roughly $6,000 to $7,000 per case as more procedures moved outpatient. However, patient out-of-pocket costs stayed largely the same, meaning those savings were not passed on to patients. For hospitals, especially those serving higher-need populations, losing high-volume inpatient procedures may create financial challenges. For taxpayers, the impact is less clear; if Medicare pays substantially less for outpatient care, the gains could be real, but if volume increases offset per-procedure savings, the net impact may be modest.
Chen: This project grew out of a broader interest in how policy changes and system shocks can reshape care delivery and provider decision-making. The COVID-19 pandemic created a unique situation where elective surgeries were suddenly paused, forcing hospitals and surgeons to rethink where and how care was provided. While we knew overall volumes dropped, much less was understood about whether the shift toward outpatient care would last and who might be left behind. In our data, we saw not only durable shifts to outpatient settings but also emerging socioeconomic differences in who received care, which raised important questions about access and equity.
Chen: Our study draws on claims from a single commercial insurer in southeastern Pennsylvania, which limits generalizability to other regions, payer types, and care settings. In particular, it excludes traditional Medicare, Medicaid, and uninsured patients — the groups most likely to face barriers to outpatient care and among whom disparities may be most pronounced. Also, because this is a descriptive study, we cannot attribute observed trends solely to the pandemic, given simultaneous policy changes and evolving provider preferences.
Chen: As the outpatient shift continues, policymakers should monitor access to outpatient surgical care among socioeconomically disadvantaged populations, as our findings suggest the benefits of outpatient migration are not evenly distributed. Payment policy should refine risk adjustment so providers are not penalized for caring for higher-need patients, and benefit design reforms should work to pass system-level savings through to patients. Investment in outpatient surgical infrastructure in underserved communities will be essential to ensuring efficiency gains do not come at the cost of equity.
Chen: This study is part of a broader research agenda focused on provider incentives and patient selection in surgical care. In my dissertation, I examined how policies like removing procedures from the inpatient-only list change both whether patients receive surgery and where they receive it, with a particular focus on substitution across procedures and patient groups. Going forward, I’m especially interested in understanding whether these shifts represent efficiency gains or reductions in access, and how they might impact health outcomes.
The study, “Inpatient to Outpatient Shifts in Surgical Care: Persistence of COVID-19 Era Changes and Socioeconomic Variations,” was published in Medical Care Research and Review on December 6, 2025. Authors include Angela T. Chen, Philip A. Saynisch, Hummy Song, Aaron Smith-McLallen, Guy David, and Alon Bergman.


Expert Insights

Replacing Flawed Current Payment Methods With the Machine Learning Model “Franklin,” Might Thwart Upcoding and Favorable Enrollee Selection by Medicare Advantage Firms

A First-of-Its-Kind Pilot Raises Safety Risks and Questions About Who Should Regulate Machines Acting Like Doctors

LDI Fellows Weigh in on the HBO Max Show, Describing Real Challenges From High Patient Bills to Assaults on Nurses in the ER
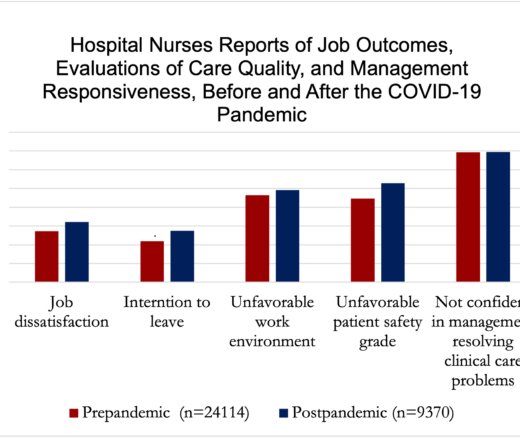
Chart of the Day: National Study Shows Worse Nurse Job Satisfaction and Perceived Lower Care Quality as Staffing Shortages Persist Post-Pandemic
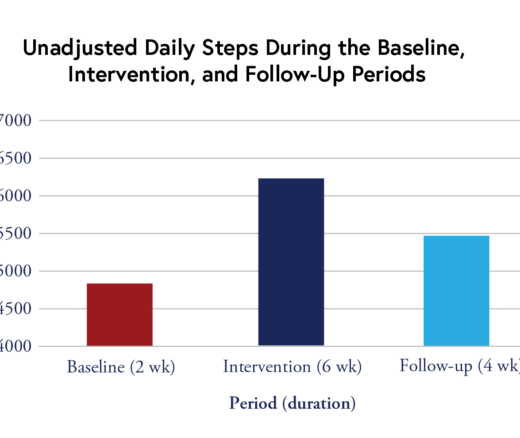
Chart of the Day: Remote Intervention with Gaming Elements Shows Promise, LDI Expert Finds