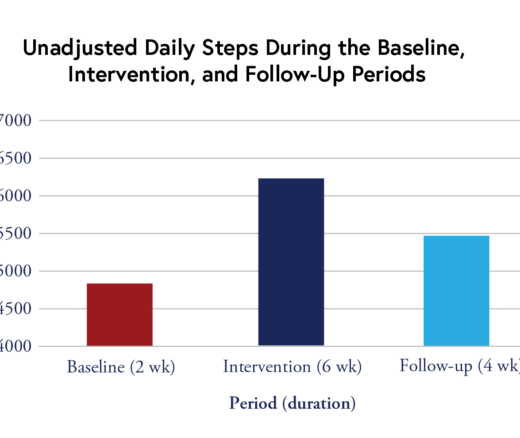
A Simple, Gamified Program Boosted Walking in Parkinson’s Patients
Chart of the Day: Remote Intervention with Gaming Elements Shows Promise, LDI Expert Finds
Improving Care for Older Adults
Blog Post

In residency, I treated an older patient with abdominal pain. A spry 80-year-old, she presented to the emergency department (ED) complaining of discomfort in her abdomen. Surrounded by family, she explained that the pain was so minimal that she did not think she needed to see a clinician. She had no other symptoms, nor any tenderness. My attending ordered a computed tomography (CT) scan anyway. It showed a large quantity of free air—evidence of intestinal perforation. After a long discussion with her family and care team, she decided not to undergo surgery and to enroll in hospice.
Older adults with abdominal pain are at much higher risk of complications and significant disease than younger patients, so much so that we might as well consider it a different phenomenon. Yet abdominal pain in older patients, which predicts morbidity and mortality at least as high as chest pain, has not received the same attention. Until recently, we didn’t even know how it was managed compared to other diseases.
Chest pain became a model system for key health economics studies that shaped what we know about value and quality in the health system. Inspired by decades of research, clinical innovation, and clinical care pathways for chest pain, our team is working to understand the status quo in geriatric abdominal pain and push care towards the future.
Thanks to LDI pilot funding, our team was able to examine how abdominal pain is managed in EDs nationally today. Our findings, published in the Journal of the American Geriatrics Society, suggest that there’s much room for improvement.
Abdominal pain accounts for 7% of all ED visits for older adults, or 7.5 million ED visits per year. On arriving, these patients were half as likely to be triaged to the “emergent” triage category as those with non-abdominal pain chief complaints, suggesting that the seriousness of their condition was underestimated by even the experienced nurses who typically run triage. This estimation doesn’t seem to be entirely correct—older adults with abdominal pain were more than four times as likely to have emergency surgery as older adults without abdominal pain, and no less likely to die or be admitted to the ICU.
In addition, 40% of older adults with abdominal pain didn’t receive a CT or ultrasound during their ED visit. These tests can help diagnose disease that may need surgical intervention. About 60% did not receive an EKG, which can help diagnose atypical heart attack symptoms and help guide other testing and treatment. And 1 in 6 received only an x-ray, which frequently shows that there are no problems even when devastating disease is brewing. What about the “pain” part of this presentation? Nearly half of older patients with abdominal pain did not receive any pain medicine, even Tylenol.
While we don’t know what the right level of testing is, these findings suggest that more clinical attention, guideline development, and research needs to be focused on this high-risk moment in the lives of many older adults.
Still, we’re a long way off from truly understanding this disease presentation. For one, we don’t know how much of the abdominal pain is chronic compared to truly acute. Are the underlying disease processes associated with abdominal pain minute-by-minute sensitive, or is a delay of an hour or two acceptable? What about 8+ hour delays that occur with increasing frequency in this post-third-wave COVID era? And how does care differ for our most vulnerable patients—those who have been shown over and over again to receive fewer resources in the health system and have poorer outcomes, such as people with disabilities or cognitive impairments, or disadvantaged minorities?
Our group hopes to answer some of these questions in future work, to inspire other groups to take acute abdominal pain in older adults seriously as a model system as important as chest pain, and to drive clinical recognition and care improvements around this geriatric chief complaint.
The study, Evaluation and Disposition of Older Adults Presenting to the Emergency Department With Abdominal Pain, was published in the Journal of the American Geriatrics Society on October 10, 2021. Authors include Ari B. Friedman, Angela T. Chen, Rachel Wu, Norma B. Coe, Scott D. Halpern, Ula Hwang, Rachel R. Kelz, and Anne R. Cappola.


Chart of the Day: Remote Intervention with Gaming Elements Shows Promise, LDI Expert Finds

Penn LDI Panel Cites Costs for Enrollees Alongside Billions in Overpayments and Systemic Gaming

New Evidence Undercuts Industry Warnings and Supports the Case To Restore Federal Minimum Staffing Standards

Washington State’s First-in-the-Nation Insurance Plan Begins Payouts in Mid-2026, and Researchers Will Weigh its Effect on Care, Costs, and the Long-Term Care Markets

Issue Brief: Understanding Gaps and Opportunities to Advance Research and Policy

An LDI Fellow Draws on Historic, Paradigm-Shifting Treatments in Depression and Obesity to Consider What Meaningful Breakthroughs in Dementia Care Could Look Like